- Visibility 47 Views
- Downloads 8 Downloads
- DOI 10.18231/j.ijor.2023.005
-
CrossMark
- Citation
Comparative outcomes between adductor canal block versus periarticular nfiltration in management of post-operative total knee replacement analgesia
- Author Details:
-
Zulfikar M Patel *
-
Himalaya Baldev
-
Nishil Patel
-
Parakhiya Brijesh Vinodbhai
-
Neel Yogeshkumar Patadia
Introduction
Total knee arthroplasty (TKA) is a gold standard surgical procedure for patients with end-stage knee osteoarthritis and rheumatoid arthritis1. Usually, patients who underwent TKA had intense moderate to severe postoperative pain and difficulty, which seriously affected life quality and postoperative rehabilitation. Early postoperative mobilization is necessary for both reduction of immobility related complications and achieving the optimal functional outcome following surgery.[1], [2], [3], [4], [5] Effective postoperative analgesia epidural analgesia also associated with unintended motor blockade, dysfunction in bowel and bladder activity, and hemodynamic instability while NSAIDS, opioids , and nonopioids medications have their own side effects in most elderly patients undergoing TKA surgery, therefore peripheral nerve block technique combined with multimodal analgesia is more preferred and emerging method of postoperative analgesia after TKA.[6], [7]
In recent times adductor canal block at the mid part of the thigh is being preferred over femoral nerve block at the groin with the benefit of maintain a sensory block for pain equivalent to femoral nerve block while minimizing motor nerve block to the Quadriceps mechanism thereby allowing early mobilization. The usage of ultrasound guidance increases the success rate of block and further reduces the risk of neurovascular injury. [8], [9], [10], [11], [12], [13], [14], [15]
Material and Methods
After obtaining institutional ethical committee approval and written informed valid consent, a study in 40 patients of either sex, ASA I/II in the age group of 40-60 years was conducted.
Study design
This is a prospective, randomized, interventional Study. It was done at Civil hospital, Ahmedabad from August 2022 to February 2023. The study drug is in government supply, and if not then the entire cost of study drugs will be bear by me. Patients who were undergoing Total Knee Replacement were divided into two groups, 20 patients in each group.
Group ACB: 0.2 % Ropivacaine 20ml.
Group LIA: 0.2% Ropivacaine 20 ml, buprenorphine (0.5ml), ketorolac (1ml) Triamcinolone 40mg (1ml) and distilled water 40 ml.
Inclusion criteria
Patients belonging to ASA grade I and II.
Patients of either sex, between the age group 40 to 60 years.
Patients with knee osteoarthritis, posted for surgery under sub-arachnoid Block.
Patients who give a valid informed and written consent.
Exclusion criteria
Contraindication for peripheral nerve or neuraxial blockade.
Patients belonging to ASA grade 3 or 4.
History of allergy to drugs implicated in this study.
Patients with infection over the injection site.
Patients who will be administered with supplementary epidural or general anaesthesia. (In patients with prolonged surgeries when conversion is required).
Patients on previous opioid therapy.
Morbid obesity.
Patients who decline consent.
Aductor canal block
The adductor canal also called as sub-sartorial block is a largely motor sparing block, anaesthetizing the femoral nerve after most of its motor branches to quadriceps have already exited, providing analgesia and Anaesthesia intraoperatively and postoperatively for surgeries to the anterior part of the knee like patellar surgery, knee arthroscopy, MCL and ACL reconstruction.
The Adductor canal is just proximal to where the femoral artery “dives” posteriorly and the probe should be positioned perpendicular to artery. At this point the femoral artery should start to pass deeper to form the popliteal artery. The vastus medialis muscle lies anterolateral, the adductor magnus muscle posteromedial and the sartorius muscle medial. Use an in- plane approach from lateral to medial ensuring that your needle tip can be seen at all times. Advance your needle into the adductor canal. This can be achieved by traversing sartorius or vastus medialis. Aspirate and inject a test dose of 1 ml of the local anaesthetic solution.
Administer 20 ml of 0.2% ropivacaine in adductor canal with negative aspiration every 5mls. Ok.
Adductor canal beneath sartorius and Site of drug deposition.
Complications
Motor block of anterior thigh.
Block failure.
Nerve Injury.
Arterial puncture, bleeding, bruising.
Intra vascular injection/ Local Anaesthetic Systemic Toxicity.
Infection.
Local intraarticular cocktail regimen infiltration
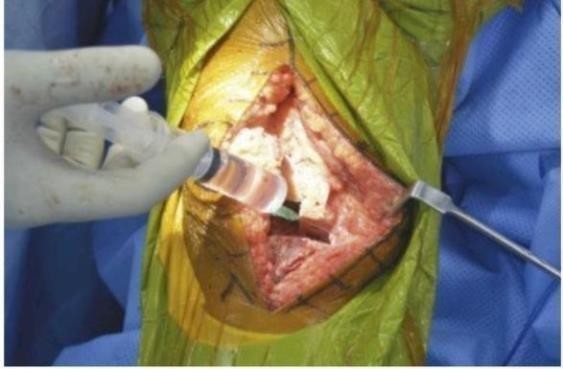
The LIA cocktail, prepared by an anesthesiologist composed of 0.2% Ropivacaine 20 ml, Buprenorphine (0.5ml), ketorolac (1ml), Triamcinolone 40mg (1ml) and distilled water 40 ml. After implantation of the component and lavage of the surgical site completed, 60 ml of LIA cocktail was given to group LIA involved in the study. The infiltration was performed using a 21-gauge needle and syringe with 8-10ml of LIA in each zone.
The cocktail was injected at the following 7 anatomical zones: Zone 1: medial retinaculum.
Zone 2: Medial collateral ligament and medial meniscus capsular attachment Zone 3: posterior capsule.
Zone 4: Lateral collateral ligament and lateral meniscus capsular attachment. Zone 5: lateral retinaculum.
Zone 6: Patellar tendon and fat pad.
Zone 7: Cut ends of quadriceps muscle and tendon.
Observation and Results
After Adductor canal block vs local intraarticular cocktail regime infiltration Results were compared using visual analogue score (VAS).
Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) score 3) Knee Society Score (Knee score and functional score).
We took 40 patients included in the study (20 each in Group ACB and Group LIA each).
Data analysis
All observations will be recorded, and results will be analyzed statistically. Data will be entered in Microsoft Excel and analyzed using student’s “t” test. Numerical data will be expressed as mean ± SD. P value < 0.05 will be interpreted as clinically significant.
|
Group Mean |
Age |
|
ACB. |
53.3 |
|
LIA |
54.45 |
[Table 1] shows mean age of patients of Group ACB is 53.3 years while that of LIA is 54.5 years. . There was no significant difference between the groups in terms of Age (Years) (p = 0.448).
|
Group. Sex |
Male Count % |
ACB.945 |
LIA 840 |
|
|
Female |
|
|
|
|
Count |
11 |
12 |
|
|
% |
55% |
60% |
[Table 2] Shows ACB AND LIA groups were comparable in terms of gender distribution. No significant difference was observed between two groups in terms of GENDER distribution.
|
1 |
Count. |
ACB.5. |
LIA 3 |
|
|
% |
25% |
15% |
|
II |
Count |
15 |
17 |
|
|
% |
75% |
85% |
[Table 3] shows ACB and LIA groups were comparable in terms of ASA grading.
|
|
ACB |
LIA |
P value |
|
Preop |
80.9±3.007 |
79.35±4.14 |
0.183 |
|
Postop-8 hrs. |
75.5±5.405 |
70.75±4.416 |
0.003 |
|
24 hrs. |
65.4±4.53 |
66.4±4.500 |
0.488 |
|
48 hrs. |
59.5±6.18 |
61.5±3.57 |
0.218 |
WOMAC score at preop: Mean score in ACB group was 80.9 and 79.35 in LIA group. P value was 0.183 which was not statistically significant.
WOMAC score at postop 8hrs: Mean score in ACB group was 75.5 and 70.75 in LIA group. P value was 0.003 which is statistically significant.
WOMAC score at postop 24hrs:
Mean score in ACB group was 65.4 and 66.4 in LIA group. P value was 0.488 which
KSS score at preop: Mean score in ACB group was 44.4 and 43 in was not statistically significant.
LIA group. P value was 0.17 which was not statistically significant.
WOMAC score at postop 48hrs: Mean score in ACB group was 76 and was 59.5 and 61.5 in LIA group. P value was 0.218 which 75.1 in LIA group. P value was 0.33 which was not statistically was not statistically significant.
|
|
ACB |
LIA |
P Value |
|
Preop |
5±0.97 |
5.1±1.25 |
0.77 |
|
Postop-8hrs. |
1.7±0.97 |
2.55±0.88 |
0.0065 |
|
24hrs. |
3.2±1.105 |
3.55±0.604 |
0.22 |
|
48hrs |
4.8±0.820 |
5±0.812 |
0.443 |
VAS score at preop: Mean score in ACB group was 5 and 5.1 inLIA group.
P Value was 0 77 which was not statistically significant
VAS score at postop 8hrs: Mean score in ACB group was KSS (functional score) at preop: Mean score in ACB was 53.07 1.7 and 2.55 in LIA group. P value was 0.0065 which is and 57 in LIA group. P value was 0.144 which was not statistically statistically significant.
VAS score at postop 24hrs: Mean score in ACB group was KSS score at postop 48hrs: Mean score in ACB group was 53.3 and 55.25 in LIA group. P value was 0.479 which was significant
VAS score at postop 48hrs: Mean score in ACB group was thus concluded that Adductor canal block in comparison with 4.8 and 5 in LIA group. P value was 0.443 which was not periarticular local infiltration provides better pain relief, good statistically significant. Range of motion, quicker rehabilitation, and reduced opioid consumption.
|
Groups |
Mean |
SD |
P Value |
|
|
ACB |
15.9 |
1.68. |
<0.001 |
|
|
LIA |
13.05 |
1.234. |
<0.001 |
|
|
Preop |
|
ACB |
LIA |
P value |
|
|
|
53.07±7.04 |
57±6.766 |
0.1444 |
|
48hrs |
|
53.5± 7.96 |
55.25±7.5 |
0.479 |
Discussion
Total knee arthroplasty (TKA) is widely performed surgery and the patients in postoperative period after TKA experiences extreme pain. An optimal analgesic regimen for patients undergoing TKA provides adequate pain management while not limiting the patient’s ability to ambulate.
Postoperative pain is often overlooked with up to 70% of patients reporting moderate to severe pain following surgery. Pain control is of prime importance in improving the quality of patient care. Regional nerve block techniques offer superior postoperative pain relief and facilitates early ambulation and discharge. Ultrasound guided blocks enables accurate placement of needle thereby improving the success rate.
Acute postoperative pain following Total Knee Arthroplasty is maximum during the first 24 hours. Various modalities have been adopted to reduce this post-operative pain with NSAIDs, parenteral opioids, central neuraxial analgesia, femoral nerve block, ACB and LIA with varying results. Among these techniques ACB block and LIA are effective and easy to perform with least complications.
Therefore, here in our prospective randomized interventional study we have compared analgesic effect of adductor canal block over local intraarticular cocktail regimen on postoperative pain and functional outcome after total knee arthroplasty. Total 40 patients satisfying the inclusion criteria were chosen and divided into two groups of twenty each. [16]
Group ACB: were administered ultrasound guided Adductor Canal Block with: 0.2 % Ropivacaine 20ml.
Group LIA: were administered local intraarticular regimen with 0.2% Ropivacaine 20 ml, buprenorphine (0.5ml), ketorolac (1ml) Triamcinolone 40mg (1ml) and distilled water 40 ml.
In this study we planned to test the hypothesis that USG guided ACB block would provide superior postoperative analgesia without having any negative impact on the functional outcome in comparison with local infiltration analgesia (LIA).
In the two groups, the recorded values were tabulated for Age, Gender, ASA, KSS (knee score), KSS (functional score), WOMAC score and VAS score post operatively. The result of the study was compared with the observation of other workers in the field of work taking into account for the differences as far as possible. [17]
Conclusion
We have conducted this study to evaluate efficacy of adductor canal nerve block versus peri-articular infiltration on postoperative pain and functional outcome after total knee arthroplasty.
In our Study
Regarding VAS score, the mean score at 8hrs in ACB group is 1.7 and in LIA group is 2.5. The difference is statistically significant (p=0.0065).
Regarding VAS score, the mean score at 24hrs in ACB group is 3.2 and in LIA group is 3.55. The difference is statistically not significant (p=0.77).
Regarding VAS score, the mean score at 48hrs in ACB group is 4.8 and in LIA group is 5. The difference is statistically not significant (p=0.443).
Regarding WOMAC score, the mean score at 8hrs in ACB group is 75.5 and in LIA group is 70.7. The difference is statistically significant (p=0.003).
Regarding WOMAC score, the mean score at 24hrs in ACB group is 65.4 and in LIA group is 66.4. The difference is statistically not significant (p=0.488).
Regarding WOMAC score, the mean score at 48hrs in ACB group is 59.5 and in LIA group is 61.5. The difference is statistically not significant (p=0.218).
Regarding the time for rescue analgesia, the mean time in ACB group is 15.9hrs and in LIA group is 13.05hrs. The difference is statistically significant (p <0.001).
Our randomized study proves that the efficacy of postoperative pain relief and functional outcome after Total knee arthroplasty is statistically better in Adductor Canal block group than in Local Infiltration Analgesia group.
Conflict of Interest
None.
Source of Funding
None.
References
- BS Kester, SV Minhas, JM Vigdorchik. Total Knee Arthroplasty for Posttraumatic Osteoarthritis: Is it Time for a New Classification. J Arthroplasty 2016. [Google Scholar] [Crossref]
- RS Sinatra, J Torres, AM Bustos. Pain management after major orthopedic surgery: current strategies and new concepts. J Am Acad Orthop Surg 2002. [Google Scholar]
- J E Paul, A Arya, L Hurlburt, J Cheng, L Thabane, A Tidy. Femoral nerve block improves analgesia outcomes after total knee arthroplasty: a metaanalysis of randomized controlled trials. Anesthesiology 2010. [Google Scholar]
- M H Chan, WH Chen, YW Tung, K Liu, PH Tan, YY Chia. Single-injection femoral nerve block lacks preemptive effect on postoperative pain and morphine consumption in total knee arthroplasty. Acta Anaesthesiol Taiwan 2012. [Google Scholar] [Crossref]
- BM Ilfeld, KB Duke, MC Donohue. The association between lower extremity continuous peripheral nerve blocks and patient falls after knee and hip arthroplasty. Anesth Analg 2010. [Google Scholar] [Crossref]
- BD chaurasiya. Human Anatomy Regional and Applied Dissection and Clinical: Lower Limb Abdomen and Pelvis. 2015. [Google Scholar]
- W Ferguson. Excision of the knee joint: recovery with a false joint and a useful limb. Med Times Gaz 1861. [Google Scholar]
- W C Campbell. Interposition of vitallium plates in arthroplasties of the knee. Clin OrthopRelat Res 1940. [Google Scholar]
- . MacIntosh Hemiarthroplasty of the knee using a space occupying prosthesis for painful varus and valgus deformities. J Bone Joint Surg Am 1958. [Google Scholar]
- B Walldius. Arthroplasty of the knee joint using an endoprosthesis. Acta Orthop Scand Suppl 1957. [Google Scholar] [Crossref]
- P Fenton, A Rampurada, F Qureshi. Bone Cement, its History, its properties, and Developments in it use. . [Google Scholar]
- FH Gunston. Polycentric knee arthroplasty: prosthetic simulation of normal knee movement. J Bone Joint Surg Br 1971. [Google Scholar]
- MB Coventry, GA Finerman, LH Riley, RH Turner, JE Upshaw. A new geometric knee for total knee arthroplasty. Clin Orthop Relat Res 1972. [Google Scholar] [Crossref]
- MA Freeman, SA Swanson, RC Todd. Total replacement of the knee using the FreemanSwanson knee prosthesis. Clin Orthop Relat Res 1973. [Google Scholar] [Crossref]
- CS Ranawat, J Insall, J Shine. Duo-condylar knee arthroplasty: hospital for special surgery design. Clin Orthop Relat Res 1976. [Google Scholar]
- CO Townley. The anatomic total knee resurfacing arthroplasty. Clin Orthop Relat Res 1985. [Google Scholar]
- PS Walker, C Ranawat, J Insall. Fixation of the tibial components of condy- lar replacement knee prostheses. J Biomech 1976. [Google Scholar] [Crossref]
